A Patient’s Guide to Distal Humerus Fractures of the Elbow
Elbow fractures are typically associated with trauma—a fall or motor vehicle accident are common causes. These injuries interfere with the ability of the elbow to place the hand in a functional position. While many elbow fractures in children can be treated nonoperatively, the majority of fractures in adults will require surgery
Anatomy
The elbow serves two distinct functions: 1) to bend and straighten 2) to turn the palm up and palm down. The elbow utilizes three bones in articulation to accomplish these purposes—humerus, ulna, and radius.
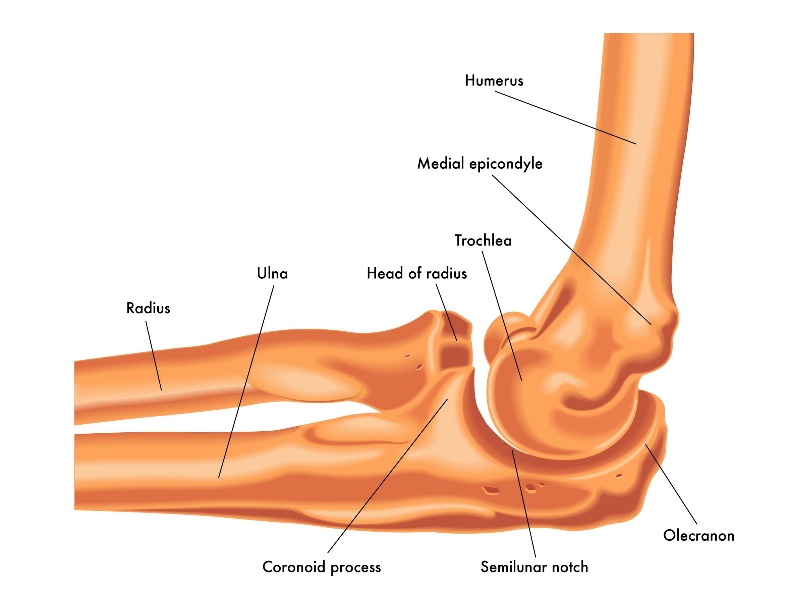
Lateral view of a right elbow demonstrating humerus, ulna, and radius
The bones of the elbow are held together by joint capsule, ligaments and tendons. As we age, the strength of both ligaments and bones decrease over time.
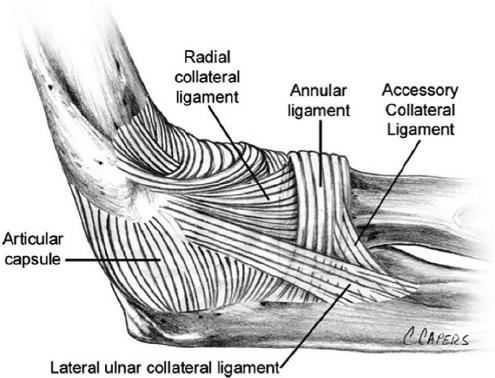
Ligaments of the elbow viewed from the lateral aspect
Diagnosis
Symptoms
Patients who experience distal humerus fractures present with pain, swelling and often bruising over time. There may be deformity of the arm dependent upon the degree of displacement of the fracture.
Physician Exam
After taking a history and noting your symptoms, a physical exam is then performed by the surgeon. The status of the vascular supply to the hand is observed. Similarly the sensation and motion of digits are noted. Although uncommon, fractures in this area may embarrass vascular supply secondary to injury or swelling. Similarly, nerve function may be disrupted due to trauma or displacement of fractures.
Imaging
X-rays are indicated to determine the bones which have been injured and if there are any dislocations associated with the injury. X-rays may be taken from several angles to better delineate the fracture.
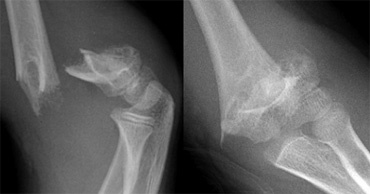
Lateral and frontal views of a comminuted supracondylar humerus fracture
In many cases, x-rays alone may adequately provide enough information to determine treatment. However, additional imaging for bone, such as computerized tomography (CT scan) may yield additional helpful information. If more concern is directed toward ligament or tendon injury, MRI imaging may be ordered.
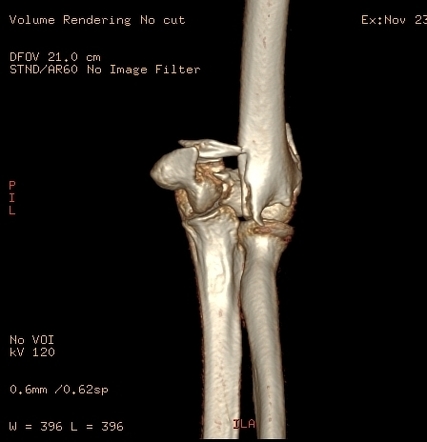
A three dimensional CT scan of a comminuted (many pieces) distal humerus fracture.
Treatment
Nonoperative
Nonoperative treatment is reserved for nondisplaced fractures currently. In the past, extensively comminuted fractures were not amenable to surgical management and therefore treated without surgery—this is rarely the case today. Nonoperative management usually requires some period of immobilization, followed by supervised range of motion. Stiffness is problematic with elbow fractures in general and may be more pronounced with longer immobilization.
Operative
Displaced fractures typically require operative management. The goals of operative treatment is to alignment the fracture and the cartilage surfaces. The cartilage surfaces are the gliding mechanism by which the elbow moves. Typically, better alignment is associated with better function.
These fractures are typically complex and require specialized care. The anesthesia choices include regional or general anesthesia. Extensile incisions may be required to place plates and screws in position. Extensive dissection to identify nerves, fracture fragments and any ligamentous injuries usually makes these procedures done in a hospital setting.
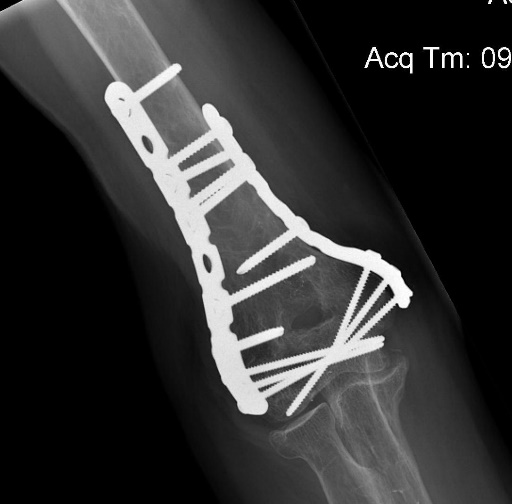
Frontal view of a distal humerus fracture treated with condylar humeral plating
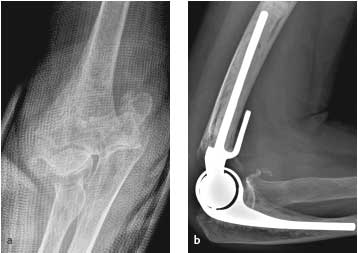
Fractures in patients with poor bone quality or extensive comminution may be candidates for elbow replacement. Front view of a comminuted elbow fracture on the left and a side view of an elbow replacement on right.
Rehabilitation
After surgery the arm is immobilized in a splint to allow for wound healing. The ability to gain stable fixation determines the amount of motion allowed for the elbow, as well as the postoperative timing. Bracing may be used in the postoperative period to control motion and formal therapy is often a useful adjuvant for care. Patients report pain after surgery, but the pain generally improves as the fracture fragments are stabilized. Initiation of therapy causes soreness for many patients.
Fracture healing requires 8-12 weeks and many patients require months of therapy to reach maximum improvement. Improvement over the injury state occurs for most individuals resulting in a functional elbow. However, even under the best of circumstances–some limitation of motion, soreness, and stiffness may result. Arthritis associated with posttraumatic arthritis may result from these severe injuries. Other complications can include infection, nerve injury, nonunion of bones, and painful hardware.


